Diabetic Foot Assessments: Why They Matter and What They Actually Involve
For anyone living with diabetes, foot health is something that deserves regular attention — not because problems are inevitable, but because early changes can be subtle and easy to miss. A diabetic foot assessment is one of the simplest, most effective ways to stay ahead of potential issues and keep your feet healthy long‑term.
Many people think of these assessments as something only needed when a problem appears. In reality, they’re most valuable before anything goes wrong.
Why Diabetes Affects the Feet
Diabetes can influence the feet in a few key ways, and each one can develop gradually:
• Reduced sensation (neuropathy)
Numbness, tingling, or altered feeling can make it harder to notice injuries.
• Reduced circulation
Slower healing and colder feet are common signs.
• Changes in skin and nails
Dryness, cracking, and thickened nails can increase risk of infection.
• Changes in foot shape or pressure
Subtle shifts in how the foot loads can lead to callus, corns, or ulcer risk.
These changes don’t happen overnight, which is why regular monitoring is so important.
What a Diabetic Foot Assessment Actually Involves
A proper diabetic foot assessment is detailed but comfortable. It’s designed to give you a clear picture of your foot health and highlight anything that needs attention.
A typical assessment includes:
Sensation testing
Checking how well you can feel light touch and vibration.Circulation check
Assessing pulses and blood flow to the feet.Skin and nail review
Looking for dryness, cracks, callus, corns, or signs of infection.Foot shape and pressure assessment
Identifying areas that may be under excess load.Footwear review
Ensuring your shoes support your foot health rather than working against it.Risk classification
Understanding whether your feet are low, moderate, or high risk — and what that means for you.
The goal isn’t to alarm — it’s to inform.
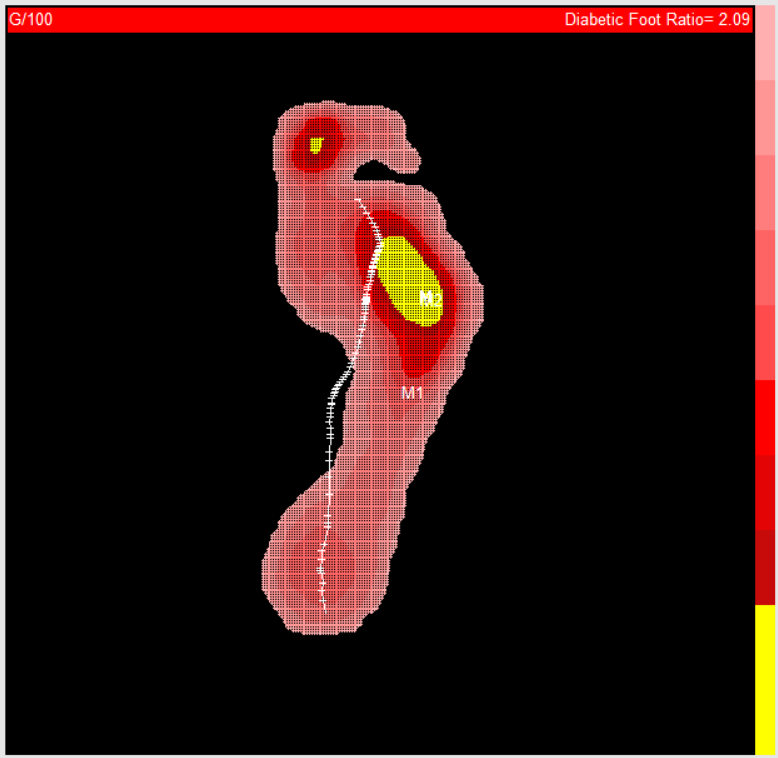
Advanced Diabetic Foot Assessment - Foot Pressure Scan - Highlighting higher pressure areas
Why Regular Assessments Matter
Even small changes can make a big difference when you catch them early.
Regular diabetic foot checks help to:
Spot issues before they become problems
Reduce the risk of ulceration
Monitor circulation and sensation over time
Identify pressure areas that may need attention
Provide reassurance and clarity
Most importantly, they give you a clear understanding of your foot health — something many people with diabetes find empowering.
How Often Should You Have a Diabetic Foot Assessment?
Most people benefit from an annual assessment, but some may need them more frequently depending on:
Sensation changes
Circulation concerns
Foot shape or pressure issues
Previous ulceration
Other health conditions
If you’re unsure, a podiatry assessment can help determine the right interval for you.
When Should You Get Checked Sooner?
It’s worth booking an assessment if you notice:
New numbness or tingling
Changes in skin colour or temperature
Hard skin that builds quickly
A blister, cut, or sore that isn’t healing
Thickened or ingrown nails
A change in how your foot feels when walking
Even small concerns are worth checking — early reassurance is always better than late intervention.
A Final Reassurance
A diabetic foot assessment isn’t about finding problems — it’s about preventing them. It’s a simple, proactive way to protect your long‑term foot health and stay confident in how your feet are doing.
If you’d like clarity on your foot health or haven’t had an assessment in a while, a diabetic foot check can give you a clear, up‑to‑date picture of what’s going on.